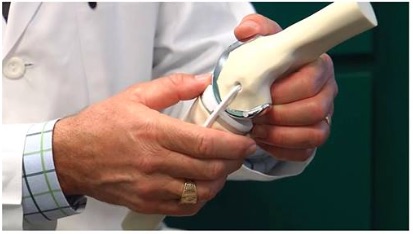
Total Knee Arthroplasty
One of the most common surgeries seen at Glen Abbey Physiotherapy in Oakville are total knee replacements (TKR), also known as total knee arthroplasties (TKA). These surgeries tend to be common for individuals that live a very active lifestyle; whether it be playing golf, soccer, racquet sports, or any other knee dominant activities. In this blog our Oakville physiotherapist will outline some indications and contraindications for surgery, what the surgery involves, what the treatment protocol is in-hospital and most importantly, what you can expect from your outpatient physiotherapists to help you reach a full recovery.
Read More About Knee Replacement Surgery Here
TKR: Before Surgery
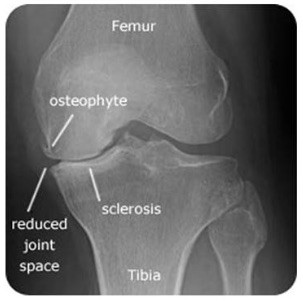 Just because you have knee pain and your neighbour across the street recently had a successful TKR does not always mean that is the right path for you. Always consult with your physiotherapist and orthopedic surgeon to decide when the best time is for your TKR and if it is indicated or not.
Just because you have knee pain and your neighbour across the street recently had a successful TKR does not always mean that is the right path for you. Always consult with your physiotherapist and orthopedic surgeon to decide when the best time is for your TKR and if it is indicated or not.
Good candidates for TKR surgery include individuals over the age of 55 with a history of moderate to severe osteoarthritis in the knee joint (most commonly the inside portion of the knee joint known as your medial compartment). Other indications include individuals with a history of rheumatoid arthritis, trauma to the knee joint itself, and/or a history of a previous TKR.
Recognize that all TKR have different life spans depending on many factors. These factors include the individual’s age, weight, activity level, sport, and type of surgical material used in the surgery. The general rule of thumb with today’s prosthetic parts are that the material will wear and tear with day to day use over a period of 10-20 years. The longevity of the prosthesis is dependent on the lifestyle of the individual it is provided for.
The Potential Dreaded Wait-list…
So you’ve talked to your physiotherapist, had an appointment with an orthopedic surgeon and they have given you the green light for a TKR. But wait… there’s a months-long wait list… now what? It is important to know that if you exercise before surgery you can have a faster and easier recovery. This is because exercise helps to keep movement in the knee joint, enhance the strength of the muscles, control pain, build your knowledge on how to exercise post surgery, reduce your body weight, and improve your sleep. The best exercises to complete pre-surgery are ones that put minimal stress on the knee joint. Some of these exercises and activities are swimming, water walking/running/aerobics, cycling, the elliptical, balance exercises, and specific knee exercises prescribed by your registered physiotherapist. Always make sure to check in with your physiotherapist about a proper exercise routine including warm up and cool down. It is also important to contact your pharmacist to learn about pain medication to help control pain and swelling pre-surgery.
Find Some Knee Replacement Prep Exercises Here
TKR Surgery and the Proceeding Days
A couple of da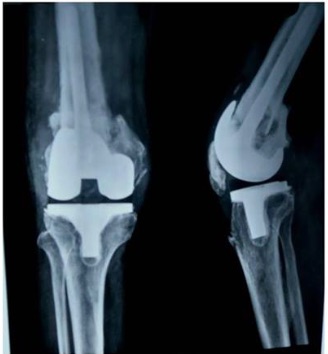 ys or weeks before your surgery you will meet with your orthopedic surgeon, physiotherapist, pharmacist, and nurse to overview the surgery and walk you through the facility. You may hear the terms ‘cemented’ or ‘uncemented’ used when the surgeon discusses your surgery. Cemented prosthetic parts use bone cement made of polycarbonate material to hold the components in place. Uncemented surgery uses a porous coating that allows for ingrowth of bone and that provides support for the implant. This method yields better revision results due to increased bone growth.
ys or weeks before your surgery you will meet with your orthopedic surgeon, physiotherapist, pharmacist, and nurse to overview the surgery and walk you through the facility. You may hear the terms ‘cemented’ or ‘uncemented’ used when the surgeon discusses your surgery. Cemented prosthetic parts use bone cement made of polycarbonate material to hold the components in place. Uncemented surgery uses a porous coating that allows for ingrowth of bone and that provides support for the implant. This method yields better revision results due to increased bone growth.
There are three major prosthetic components that make up a TKR; the femoral component (the bottom part of your thigh bone), the tibial component (the top of your shin bone), and the patellar component (the back side of your knee cap). The surgeon will perform a lateral release and detach the inner quad muscle to allow the joint to be exposed. The anterior cruciate ligament (ACL) and top part of your shinbone are removed along with your menisci and any osteoarthritis. The surgeon will then align the prosthesis so that your posterior cruciate ligament (PCL) is not impinged and that your kneecap properly tracks with your knee. The back third of the kneecap is then shaved down to allow the patella component to be attached along with the femur and tibial component.
Click To Learn More About Knee Replacement Surgery Here
From the operating room you will be moved to inpatient care within the facility. You will immediately be getting up from your bed with a physiotherapist and nurse, be assessed on your bed mobility and your ability to move from one area to another. Foot and ankle exercises are started immediately to promote blood flow and circulation throughout the limb and to help prevent any clotting from occurring post surgery. By your second day you will be ambulating with a walking aid, utilizing stairs, work on gentle range of motion exercises, and begin beginner level quad strengthening exercises. If your hospital stay is longer than the usual 1-3 days this may be due to numerous other factors including older age, delayed healing, thrombophlebitis (blood clotting), infections, blood loss, poor mobility, or antecedent medical problems occurring from any surgical operation. From here you will be discharged and begin working with a physiotherapist here at Glen Abbey physiotherapy in Oakville to assist you in your recovery.
What to Expect After Knee Replacement Surgery
 During the first three weeks it is important that you keep your knee pain and swelling under control with the use of exercise, ice, physiotherapy, acupuncture, education, and mobility exercises. It is important to get enough sleep to allow natural healing to occur. It is equally as important to focus on the exercises prescribed by your physiotherapist to improve your motion of the knee, pain, strength, and swelling. Goals within the first 3 weeks include bending your knee to 90 degrees which is the motion you have when sitting on a chair with your foot flat on the ground. Another goal is to achieve a straight knee to roughly 5-10 degrees. This would be the ability to fit 3-5 finger widths under your knee when attempting to straighten it. Our Oakville physiotherapists will work on bending and straightening your knee to improve your range of knee motion. They will provide you with a home exercise program to help restore full motion and improve your muscle strength.
During the first three weeks it is important that you keep your knee pain and swelling under control with the use of exercise, ice, physiotherapy, acupuncture, education, and mobility exercises. It is important to get enough sleep to allow natural healing to occur. It is equally as important to focus on the exercises prescribed by your physiotherapist to improve your motion of the knee, pain, strength, and swelling. Goals within the first 3 weeks include bending your knee to 90 degrees which is the motion you have when sitting on a chair with your foot flat on the ground. Another goal is to achieve a straight knee to roughly 5-10 degrees. This would be the ability to fit 3-5 finger widths under your knee when attempting to straighten it. Our Oakville physiotherapists will work on bending and straightening your knee to improve your range of knee motion. They will provide you with a home exercise program to help restore full motion and improve your muscle strength.
By weeks 3 to 6 your knee will feel improved in regards to range of motion, swelling, pain and strength. Your exercises prescribed by your physiotherapist will begin to progress in difficulty. Your physiotherapist will begin joint mobilizations to help restore the natural mobility of the knee joint. Here at Glen Abbey Physiotherapy in Oakville our team will utilize exercise, myofascial release, interferential current, ultrasound, ice, heat, shockwave, acupuncture, compression, and education amongst many other treatment interventions to get you back onto your feet. In an ideal situation, your knee will achieve 100-115 degrees of flexion and 3 degrees of extension. You will begin walking up and down stairs with a more normal motion, be able to begin stationary bike exercise and be able to sit and stand independently from a regular chair. At 6 weeks you will also meet with your orthopedic surgeon for a follow up appointment to check in on your progress.
During weeks 6 through 12 you will progress your exercises, strength, mobility, joint mobility, range of motion, swelling and manage your pain with your physiotherapist. Remember that you may find pain and swelling increase as you begin new exercises and improve your movement. Everyone heals differently and the timetable to meet and exceed post-surgical goals differs from person to person. Always talk with your physiotherapist and surgeon if you feel as though you are not meeting your goals in a timely manner.
Our physiotherapists always include a home exercise program as part of their physical therapy treatment. In the beginning, post operative exercises are simple and often involve moving the foot and knee to manage swelling and encourage blood flow. Gradually exercises will be introduced to slowly bend the knee and you will start muscle strengthening exercises like straight leg raises. The exercise guidelines will be detailed by our physiotherapists including instructions on number of repetitions, sets and how many times a day the exercises should be completed.
Find Some Post-Surgical Knee Replacement Exercises Here
Advice for 3 months – 1 year post TKR
A good level of fitness and activity will help improve the life span of your joint replacement. Exercises helps to increase strength, range of motion, reduce the risk of falls, improve cardiovascular endurance, keep your weight under control, and improve your bone quality. Focus on flexibility exercises to help maintain the range of motion that you have gained post surgery. Stretch when you are done your exercises or even after a walk. Warmer muscles are always easier to stretch. Attempt to stretch 3-4 days per week and apply heat appropriately to help with stretching. Commit to a long term strengthening program to help regain and keep your strength to protect your joint replacement. Your operated knee will take up to a year to regain normalized strength relative to your non-operated knee. To maintain current strength, strength train 2-3 times per week. To increase your strength, strength train 3-4 times a week. Always rest the day after doing strengthening exercises to let your muscles recover. Do not attempt to strengthen the knee for more then 4 days within a single week once you are a year post surgery. Remember to also train your balance after a total joint replacement to help reduce your risk of falling. Always have a firm counter top, chair or railing to hold on to when completing your balance regime.
Here are some physical activity tips following your TKR: 
- Following a TKR it is best to follow activities, which are low impact.
- Allowed activities are: stationary cycling, road cycling, golf, swimming, walking, speed walking, hiking, canoeing, square dancing, ballroom dancing, bowling and shuffleboard.
- The following activities are normally allowed with experience: aerobics, yoga, ice skating, cross-country skiing, downhill skiing, stationary skiing, doubles tennis, horseback riding and rowing.
- The following activities are not recommended: jogging, basketball, football, soccer and volleyball.The following activities should be talked over with your physiotherapist and orthopedic surgeon: squash, racquetball, singles tennis, weight machine, roller skating, weight lifting, baseball, gymnastics, handball, hockey, rock climbing and fencing.
If there is an activity you would like to do after having a TKR which is not listed above, please come into the clinic to meet with one of our trained, registered physiotherapists. After an assessment they will be able to provide education and prescribe exercise that is suitable to your individual needs. If you have any questions or concerns about having a total knee replacement or are suffering from a knee impairment make sure to visit us here at Glen Abbey Physiotherapy! We can help you on your way to an active, complete recovery.