After any traumatic injury the first thing that is cleared by any health care professional, whether it be your Oakville physiotherapist at Glen Abbey Physiotherapy or the emergency doctor, is a fracture. If you roll your ankle while slipping on ice and cannot weight bear on your foot, when you arrive to your local emergency department an x-ray will be completed to either rule in or rule out the injury of a fracture. If a fracture is diagnosed, hundreds of questions run through a patient head about severity, long term prognosis, your activities of daily living, being braced, surgery, etc. However, having some fundamental knowledge about types of fractures and what they mean can help you greatly be prepared if and when a fracture occurs. In this blog post we will define what a fracture is, the classification of fractures, causes of fractures, signs and symptoms of a fracture, factors that influence fracture healing and the role of physiotherapy provided by your physiotherapist at Glen Abbey Physiotherapy.
Types of Fractures
So what exactly is a fracture? A fracture is a complete or incomplete disruption of the osseous integrity of a bone. The osseous tissue is a dense connective tissue made consisting of a two mineralized types of bone known as cortical and cancellous. Together, this tissue has a honeycomb like appearance allowing for the bone to be rigid and strong under forces. When this tissue is compromised and disrupted, the term ‘fracture’ is used. A fracture has a wide range of severity to it, therefore a classification system is warranted to best understand what exactly your fracture means.
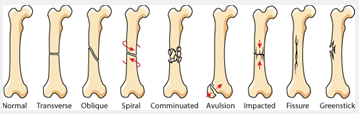
Read More About Bone Fractures Here
There are 9 main factors that help us at Glen Abbey Physiotherapy classify a type of fracture. They are as follows:
- The anatomical location of the fracture. Whether it may be to the ‘middle’ of the bone or possibly outer edge
- The direction of the fracture. This then in turn creates different type of fractures such as oblique, spiral, transverse etc.
- The mechanism of injury. Fractures may occur from overuse, whiplash associated disorders, or rolling an ankle
- Open versus closed. An open fracture (compound) is when the fracture has breached the skin – the skin may be breached externally from force or internally as the bone end pushes through soft tissue, thus infection is more likely to occur. A closed fracture (simple) on the other hand, does not break the skin and therefore is not an open wound.
- Complete versus incomplete. Incomplete fractures (greenstick fracture for example) may bend but not completely separate themselves, however a complete fracture does resulting in the bone being in 2 or more pieces.
- The angulation. This relates to whether the fracture occurred on the front, back, or side.
- The degree of apposition and overlap. Depending on the direction and angulation of the bone, when fractured it may overlay part of it’s remaining origin.
- The joint involvement. If fractures occur in close proximity to a joint or directly on the joint it must be noted as management and interventions change drastically.
- Epiphyseal involvement. The epiphyseal plate, also known as growth plate, is commonly seen in children known as a Salter-Harris type of fracture.
By understanding this classification system, you can have true insight into what your x-ray truly means when a fracture is located. For example, an x-ray may state complete open oblique fracture of the humeral shaft via fall on hand. Just from this one line, you understand the severity of the fracture, whether an infection is likely or not, the direction of the fracture, where it was, and how it occurred. Although having this knowledge doesn’t make you an x-ray technician, it sure does help you have some baseline knowledge of what exactly is happening to your bone.
How Do Fractures Occur
There are many reasons a bone can fracture. Your bone may fracture from a trauma, such as a indirect blow or a fall on an out-stretched hand. Fractures can also occur directly – such as a baseball bat to the arm or leg. They may occur from overuse or fatigue, such as a stress fracture in the foot from over running. However, some causes of fractures are pathological in nature, such as bone diseases, tumours, cancer, cysts or even other conditions such as overuse steroid therapy. These conditions all cause the bone to weaken and in the most advanced stages can lead to fractures.
Signs and Symptoms of a Fracture
In regards to trauma, overuse and pathological conditions resulting in fractures, there are some evident signs and symptoms. There will be pain, usually sharp and localized to the site of the injury. The appearance of your tissue will change; resulting in swelling, deformity and bruising. You will likely be reluctant to move the area of concern and cradling the limb is in the upper extremity. Muscle spasms will arise and tenderness to touch or vibration forces will be noted. Movement will be weak and restricted due to pain and reflex inhibition. X-rays are always the gold standard to detect a fracture, however a bone scan, CT scan or MRI may be warranted to identify more obscure fractures.
Factors That Affect Healing Time
Once a fracture is diagnosed via x-ray, you should be aware of the many factors, which influence a bones ability to heal.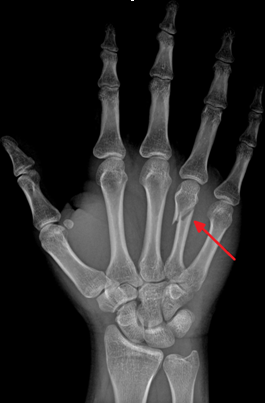
- Circulation – circulation plays a large role as bones that have inadequate circulation heal slowly. A common fracture site is at the scaphoid (a small bone in the wrist), because of its hourglass shape, if compromised in the middle of the bone, limited blood is able to get to the distal end thus causing poor circulation and in turn dies off the end of the bone known as necrosis.
- Hormones – Growth hormones may stimulate bone healing whereas large doses of cortisone may delay fracture healing. Severe dietary restrictions may decrease a bones ability to heal, if the patient has a chronic disease resulting in poor or inadequate nutrition to the body. How you rest your fracture plays a large role, if the fracture is compressed via brace or cast, this will prevent movement of the bony ends and allow the fragments to heal more readily, this is very important for burst fractures.
- Age – The age of an individual plays a large role in healing. Younger individuals heal faster then their counterparts, with increased age bones becomes less stiff, less strong and more brittle with more porous material and fewer, thinner and longer trabeculae (cancellous bone tissue).
- Type of Fracture – The site of the fracture (your upper limb heals faster then your lower limb) and shape of the fracture (a transverse fracture takes longer to heal than a spiral fracture) along with the amount of displacement of the fracture; fractures with greater displacement and comminution will take longer to heal than a simple undisplaced fracture, all play a large role in fracture healing. Infection, anemia or hypoxia may all slow fracture healing. Along with poor physical fitness and health, as low levels of vitamin C is required for normal collagen matrix formation and exercises may increase fracture healing as long as the callus is not dislodged by extreme or excessive activity.
- Bone Type – Lastly, the type of bone plays a large role in how well a bone fracture may heal, as intra-articualar (in the joint) fractures take longer to heal than extra-articular (outside of the joint line) fractures due to the presence of synovial fluid hindering the formation of granular tissue.
Read More About How A Fracture Heals
Physiotherapy After a Fracture
 So what can physiotherapy do to help you after a fracture is diagnosed? At Glen abbey physiotherapy, our Oakville physiotherapists are trained, registered professionals. They will identify the cause of the problem and select the appropriate procedure to alleviate or eliminate the cause of the loss of movement. We will perform a detailed assessment of the joints above and below the fracture site to understand the strength, range of motion, mobility, length tension and composition of your area of injury via objective measures. From there, a treatment program will be created to help you get back on the road to recovery. Following your initial assessment, your physiotherapist will give you exercise to help manage your condition at home via a home exercise program. They will also help educate you about the condition, utilization of any modality, positioning, bracing, prognosis and more. Treatment of a fracture truly depends on the classification system of a fracture and the type of fracture, along with recommendations by your surgeon if they are required. At Glen Abbey Physiotherapy, you can trust your physiotherapist and team to get you back to the best of your abilities, activities of daily living, and hobbies all the with understanding that each fracture is different depending on the factors of bone healing. If you or someone you know has had a recent fracture, give us a call at Glen Abbey Physiotherapy to be assessed by one of our physiotherapists.
So what can physiotherapy do to help you after a fracture is diagnosed? At Glen abbey physiotherapy, our Oakville physiotherapists are trained, registered professionals. They will identify the cause of the problem and select the appropriate procedure to alleviate or eliminate the cause of the loss of movement. We will perform a detailed assessment of the joints above and below the fracture site to understand the strength, range of motion, mobility, length tension and composition of your area of injury via objective measures. From there, a treatment program will be created to help you get back on the road to recovery. Following your initial assessment, your physiotherapist will give you exercise to help manage your condition at home via a home exercise program. They will also help educate you about the condition, utilization of any modality, positioning, bracing, prognosis and more. Treatment of a fracture truly depends on the classification system of a fracture and the type of fracture, along with recommendations by your surgeon if they are required. At Glen Abbey Physiotherapy, you can trust your physiotherapist and team to get you back to the best of your abilities, activities of daily living, and hobbies all the with understanding that each fracture is different depending on the factors of bone healing. If you or someone you know has had a recent fracture, give us a call at Glen Abbey Physiotherapy to be assessed by one of our physiotherapists.
Post Fracture Acupuncture
Managing pain and swelling can be an important initial phase of the treatment process. Acupuncture can help! Our Oakville acupuncture provider, Dr. Jenn, uses acupuncture to flush away swelling, speed up healing and decrease the overall pain you are experiencing. Acupuncture is painless, and is an excellent adjunct to physiotherapy treatment. Acupuncture treatments typically last 20-30 minutes, and can drastically help reduce pain and improve overall function.